The human immune system is often misunderstood as a static shield, a predetermined defense mechanism gifted or withheld by genetics. In reality, immunity is an active, dynamic surveillance state. It is a highly sensitive network of cells, tissues, organs, and chemical messengers that is entirely dependent on the environment you create for it. While pathogens are the external threats, the internal terrain dictates whether those threats are neutralized or allowed to multiply.
Modern life is fundamentally mismatched with our evolutionary biology. The habits we have normalized—eating out of boxes, sacrificing sleep for productivity, chronic psychological stress, and moving less—are not merely “unhealthy” in a vague sense. They actively dismantle the immune system at a cellular and molecular level.
This deep dive explores the precise, scientifically documented mechanisms through which modern lifestyle habits destroy your immunity, and what the latest clinical data reveals about reversing the damage.
1. The Dietary Saboteurs: Ultra-Processed Foods and the Gut Microbiome
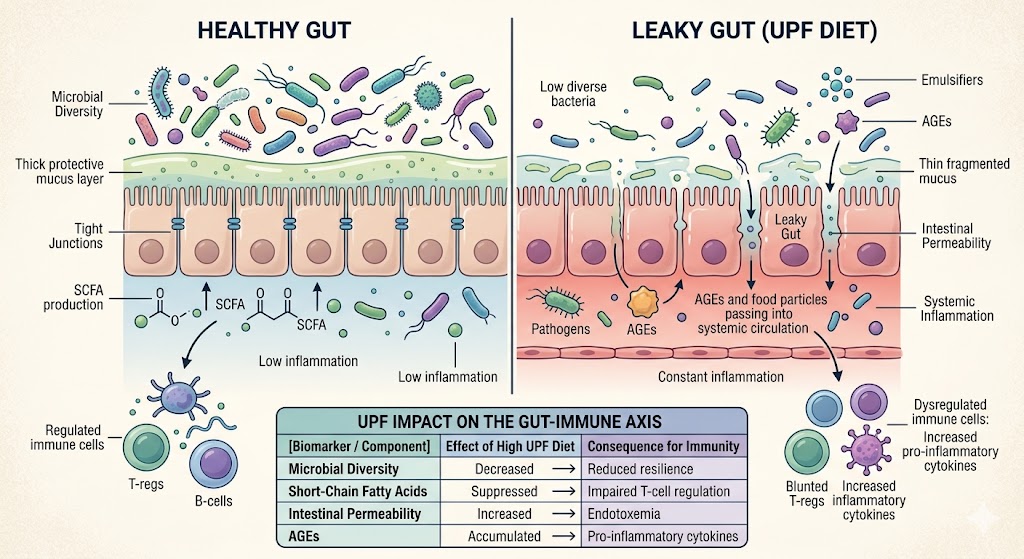
The gastrointestinal tract houses roughly 70% of the immune system. The gut lining is a single layer of epithelial cells separating the systemic circulation from trillions of microbes and food particles. How you feed this ecosystem directly dictates your immune competence.
The Rise of Ultra-Processed Foods (UPFs)
Ultra-processed foods (industrial formulations of food derivatives, artificial flavors, and chemical additives) have become the default diet for much of the developed world. Research published in Frontiers in Immunology and MDPI clearly outlines how UPFs induce immune dysregulation.
UPFs are typically devoid of dietary fiber but rich in Advanced Glycation End products (AGEs), refined sugars, and saturated fats. When you consume UPFs, you are starving the beneficial gut bacteria that rely on complex carbohydrates to produce Short-Chain Fatty Acids (SCFAs) like butyrate. SCFAs are critical signaling molecules that regulate regulatory T-cells (Tregs), which prevent the immune system from attacking the body’s own tissues.
Emulsifiers and the “Leaky Gut” Phenomenon
Beyond macronutrient profiles, the chemical additives in UPFs actively degrade immune defenses. Emulsifiers such as polysorbate-80 and carboxymethyl cellulose—used to improve texture and shelf-life—have been clinically shown to strip away the protective mucus layer of the intestines.
When this barrier is compromised, it leads to increased intestinal permeability (often termed “leaky gut”). Pathobionts (opportunistic bacteria) and undigested food particles slip through the epithelial barrier into the bloodstream. The immune system flags these as foreign invaders, triggering a constant, low-grade systemic inflammatory response.
Data Breakdown: UPF Impact on the Gut-Immune Axis
| Biomarker / Component | Effect of High UPF Diet | Consequence for Immunity |
| Microbial Diversity | Significantly Decreased | Overgrowth of pathogenic bacteria (e.g., Clostridium); reduced resilience. |
| Short-Chain Fatty Acids | Suppressed | Impaired T-cell regulation; increased risk of autoimmune responses. |
| Intestinal Permeability | Increased | Endotoxemia; chronic systemic inflammation. |
| Advanced Glycation End Products (AGEs) | Accumulated | Binds to RAGE receptors on immune cells, triggering pro-inflammatory cytokines. |
When the immune system is locked in a state of chronic, low-grade inflammation due to diet, its resources are depleted. If a genuine viral or bacterial threat enters the body, the immune response is delayed, disorganized, and less effective.
2. The Sleep Crisis: The Biological Cost of the All-Nighter
There is a cultural tendency to view sleep as a luxury or a flexible commodity. Biologically, sleep is a non-negotiable metabolic and immunological reset. The science of sleep and immunology reveals a strictly bidirectional relationship: your immune system dictates how you sleep, and how you sleep dictates your immune function.
The Glymphatic Clearance System
In 2013, neuroscientists discovered the glymphatic system, a macroscopic waste clearance pathway in the central nervous system. During deep, slow-wave sleep, the brain’s glial cells shrink, allowing cerebrospinal fluid to wash rapidly through brain tissue. This process flushes out metabolic debris, including immune-active substances and neurotoxins.
When sleep is truncated, the glymphatic system fails to clear this debris, leading to neuroinflammation. This inflammation directly affects the suprachiasmatic nucleus (SCN) in the hypothalamus—the brain’s master clock—creating a vicious cycle of further sleep disruption and immune dysfunction.
T-Cell Adhesion and Cytokine Production
During the early hours of sleep, the immune system undergoes a massive redistribution. The production of certain pro-inflammatory cytokines peaks, acting as a signaling mechanism to help the body “remember” previously encountered pathogens.
More importantly, a lack of sleep actively impairs T-cell function. T-cells are the “special ops” of the adaptive immune system, responsible for identifying and destroying virus-infected cells. To destroy a target, a T-cell must adhere to it using proteins called integrins. Research indicates that sleep deprivation directly reduces integrin activation. A tired T-cell is physically less capable of latching onto and neutralizing a viral threat.
Charting the Sleep-Immune Cycle
The Bidirectional Feed-Forward Loop of Sleep Deprivation
[Poor Sleep Quality / Insomnia]↓ leads to
[Reduced Glymphatic Clearance & T-Cell Integrin Activation]↓ leads to
[Increased Systemic & Neuroinflammation]↓ leads to
[Hypothalamus/SCN Disruption]↓ leads to
[Heightened Wakefulness & Worse Sleep Architecture]
Clinical polysomnography data consistently shows that individuals with higher perceived stress and sleep latency (taking longer than 15-20 minutes to fall asleep) exhibit sleep efficiency below 85%. This fragmentation drops natural killer (NK) cell activity—the frontline defenders against tumors and viruses—by up to 70% after just a single night of restricted sleep (e.g., 4 hours).
3. Chronic Stress: The HPA Axis and Glucocorticoid Resistance
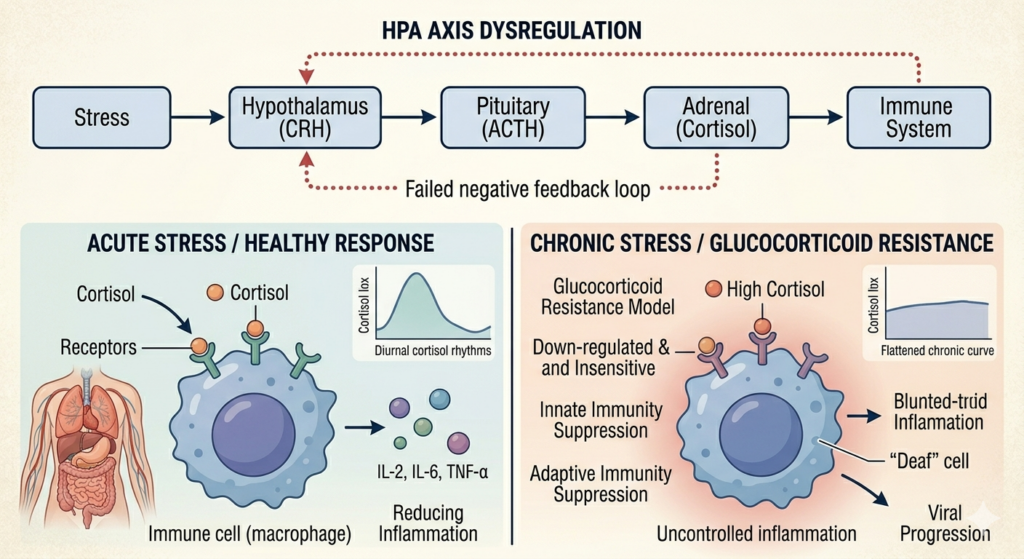
Occasional stress is a survival mechanism. Chronic psychological stress—worrying about finances, career pressures, or relationships—is a modern invention that short-circuits the neuroendocrine system.
The Hypothalamic-Pituitary-Adrenal (HPA) Axis
When you perceive a threat, the HPA axis activates. The hypothalamus releases corticotropin-releasing hormone (CRH), signaling the pituitary gland to release adrenocorticotropic hormone (ACTH), which finally tells the adrenal glands to pump out cortisol and catecholamines (adrenaline and noradrenaline).
In healthy adults, cortisol production averages 8 to 30 mg per day, following a diurnal rhythm that peaks in the morning. During acute stress, a spike in cortisol is actually anti-inflammatory. It suppresses immune activity to ensure the body’s energy is diverted toward immediate survival (the “fight or flight” response).
The Glucocorticoid Resistance Model
The biological disaster occurs when stress never ceases. If cortisol levels remain perpetually elevated due to a high-stress lifestyle, the immune system must adapt to survive the constant hormonal bombardment. It does this by downregulating its glucocorticoid receptors.
This phenomenon is known as Glucocorticoid Resistance. The immune cells effectively become “deaf” to cortisol’s anti-inflammatory signals. Because cortisol can no longer apply the brakes, the immune system remains locked in an inflammatory state.
- Innate Immunity Suppression: High cortisol directly interferes with Toll-like receptor signaling in macrophages, blinding them to incoming pathogens.
- Adaptive Immunity Suppression: Cortisol inhibits the expression of vital interleukins (IL-2, IL-6) and Tumor Necrosis Factor-alpha (TNF-a), preventing T-cells and B-cells from communicating effectively.
- Viral Progression: Clinical studies mapping the immune response of individuals under cronic stress (such as caregivers for spouses with dementia) demonstrate a significantly blunted antibody response to vaccines and a higher severity of symptoms when exposed to rhinoviruses (the common cold).
The Neurotransmitter Connection: Serotonin and Dopamine
Stress does not just alter cortisol; it disrupts your neurotransmitters, which are intimately linked to immune function. Approximately 90% of the body’s serotonin is produced in the gut. During chronic stress, serotonergic and dopaminergic activation forces a miscommunication between the central nervous system and the immune system. Immune cells possess dopamine and serotonin receptors; abnormal fluctuations in these neurotransmitters directly suppress the aggressive action of lymphocytes and macrophages.
4. The Physical Activity Paradox: Sedentary Atrophy vs. Overtraining
Movement is the engine of the lymphatic system. Unlike the cardiovascular system, which has a pump (the heart) to circulate blood, the lymphatic system relies entirely on muscle contraction and physical movement to circulate lymph fluid. This fluid carries white blood cells throughout the body to hunt for infections.
The Sedentary Lifestyle
Sitting at a desk for eight to ten hours a day causes lymphatic stagnation. Without muscular contraction, the surveillance capacity of the immune system drops drastically. A sedentary lifestyle also promotes visceral fat accumulation. Adipose (fat) tissue is not inert; it is highly biologically active. Visceral fat continuously secretes pro-inflammatory cytokines called adipokines. This creates a baseline of systemic inflammation that exhausts immune reserves, leaving the body vulnerable when a true pathogen arrives.
The Danger of Overtraining
At the opposite end of the spectrum is the overtraining syndrome. While moderate exercise dramatically enhances immune function by temporarily increasing the circulation of immunoglobulins and neutrophils, extreme physical stress without adequate recovery does the exact opposite.
Endurance athletes or fitness enthusiasts pushing their limits daily without rest induce an “open window” of altered immunity. High-intensity, exhaustive exercise causes a massive spike in adrenaline and cortisol, paired with severe oxidative stress and muscle micro-tears. In the hours following such exertion, the body’s immune defenses are actively suppressed to prevent an autoimmune reaction to the damaged muscle tissue. If lifestyle habits do not allow for recovery, this “open window” becomes a permanent draft, inviting frequent upper respiratory tract infections.
5. Toxins in Plain Sight: Alcohol, Smoking, and Vaping
The introduction of socially acceptable toxins provides a direct, physical assault on the mucosal barriers of the immune system. The respiratory and digestive tracts are lined with specialized immune cells and physical barriers designed to trap and expel invaders.
Alcohol: Breaching the Barrier
Alcohol consumption, particularly binge drinking, alters the immune system in several profound ways.
- Microbiome Devastation: Alcohol acts as a solvent, indiscriminately killing gut bacteria and altering the microbiome composition.
- Liver Impairment: The liver is central to immunity; it produces acute-phase proteins and clears bacteria from the bloodstream. When the liver is busy metabolizing ethanol, its immunological functions are sidelined.
- Ciliary Paralysis: In the lungs, microscopic hair-like structures called cilia sweep pathogens upward and out of the airway. Alcohol directly paralyzes these cilia, significantly increasing the risk of pneumonias and respiratory infections.
Smoking and Vaping: Oxidative Devastation
Smoking combustible tobacco introduces thousands of free radicals into the pulmonary tissue. This oxidative stress overwhelms the local immune defense, destroying the structural integrity of the lung tissue.
Vaping, often incorrectly viewed as a harmless alternative, introduces a different kind of threat. The aerosolized propylene glycol, vegetable glycerin, and flavorings severely impair the function of alveolar macrophages—the “pac-man” cells of the lungs that swallow dust and bacteria. Studies demonstrate that e-cigarette vapor causes macrophages to become sluggish, failing to clear out infectious agents effectively.
6. The Modern Plague: Social Isolation and Loneliness
Perhaps the most insidious, yet scientifically fascinating, lifestyle factor destroying immunity is social isolation. Human beings are inherently tribal. From an evolutionary perspective, being isolated from the group meant an increased risk of predation or physical injury.
Conserved Transcriptional Response to Adversity (CTRA)
Genomic researchers have identified a specific gene expression profile triggered by chronic loneliness and social isolation, known as the Conserved Transcriptional Response to Adversity (CTRA).
When the brain perceives social isolation, it shifts the immune system’s genetic expression to prepare for physical trauma (which, historically, was the greatest threat to a solitary human).
- Upregulation: The body turns up the genes responsible for inflammation to heal wounds and fight bacterial infections from animal bites.
- Downregulation: The body turns down the genes responsible for fighting viral infections (since you are not around other humans, the evolutionary risk of catching a virus is low).
Living a highly isolated lifestyle literally rewires your DNA expression to turn off your antiviral defenses while keeping you in a state of chronic, damaging inflammation.
Conclusion: Rebuilding the Defense System
Your immune system is a reflection of your daily behaviors. Recognizing that lifestyle habits can destroy immunity is the first step; the second is understanding that the damage is largely reversible.
The biological mechanisms outlined above—gut dysbiosis from ultra-processed foods, neuroinflammation from sleep deprivation, glucocorticoid resistance from chronic stress, and lymphatic stagnation from immobility—are not life sentences. They are dynamic states.
To rebuild immunity, the scientific consensus points away from “miracle supplements” and toward foundational biological alignment:
- Prioritize the Microbiome: Shift away from emulsifiers and refined sugars. Focus on diverse, fiber-rich whole foods to support the production of short-chain fatty acids.
- Respect the Circadian Rhythm: View 7-9 hours of sleep not as rest, but as active glymphatic clearance and T-cell recalibration. Maintain a consistent sleep-wake cycle to protect the HPA axis.
- Manage Cortisol: Stress cannot be eliminated, but it must be managed to prevent glucocorticoid resistance. Mindfulness, deep breathing, and active recovery are clinical necessities, not just wellness buzzwords.
- Move Consistently, Recover Adequately: Use moderate physical activity to drive lymphatic flow, but respect the body’s need to heal oxidative stress.
By aligning your lifestyle with human biology rather than fighting against it, you stop sabotaging your cellular defenses and allow your immune system to function exactly as it evolved to do: with ruthless, precise efficiency.
References & Scientific Grounding
- National Institutes of Health (NIH) / PubMed Central: Clinical Understanding of the Sleep-Immune Connection (PMC9005150) detailing the glymphatic system and hypocretin influences.
- Frontiers in Immunology: Research on Ultra-Processed Foods and Gastrointestinal Microbiota Alterations.
- StatPearls (NCBI Bookshelf): Physiology of Cortisol, the Hypothalamic-Pituitary-Adrenal (HPA) Axis, and Glucocorticoid Resistance mechanisms.
- MDPI Biology / Nutrients: Regulation of Stress-Induced Immunosuppression in the Context of Neuroendocrine, Cytokine, and Cellular Processes; Ultra-Processed Foods and Inflammatory Bowel Disease.
- Medicine LibreTexts: Biological models of Stress and Immunity, detailing T-cell suppression and natural killer (NK) cell degradation.
